Survodutide mechanism of action : The Science Behind Survodutide (BI 456906)
1.The Era of “Synergistic Poly-Agonism”
For decades, the pharmacological management of metabolic syndrome was a game of single targets. We treated hyperglycemia with insulin or sulfonylureas. We treated obesity with simple appetite suppressants. Even the arrival of Semaglutide (a GLP-1 mono-agonist) represented a single, albeit powerful, lever: the satiety signal.
Survodutide (BI 456906) represents a fundamental shift in this paradigm. It is not merely a stronger version of what came before; it is a “molecular chimera” designed to manipulate two opposing physiological forces simultaneously. Co-developed by Boehringer Ingelheim and Zealand Pharma, Survodutide is a dual agonist targeting both the Glucagon-like peptide-1 receptor (GLP-1R) and the Glucagon receptor (GCGR).
To the uninitiated, this combination seems counterintuitive. GLP-1 lowers blood sugar; Glucagon raises it. Why combine them? The answer lies in the complex “yin and yang” of human bioenergetics. By meticulously engineering the ratio of receptor activation, Survodutide harnesses the appetite-suppressing power of GLP-1 while unlocking the “forbidden” metabolic accelerator of Glucagon: Energy Expenditure.
This deep dive explores the Survodutide mechanism of action at the molecular, cellular, and systemic levels. We will dissect how this peptide achieves weight loss figures approaching 19%, why it is being hailed as a breakthrough for liver fibrosis (MASH), and the precise intracellular cascades that allow it to burn fat while protecting the heart.
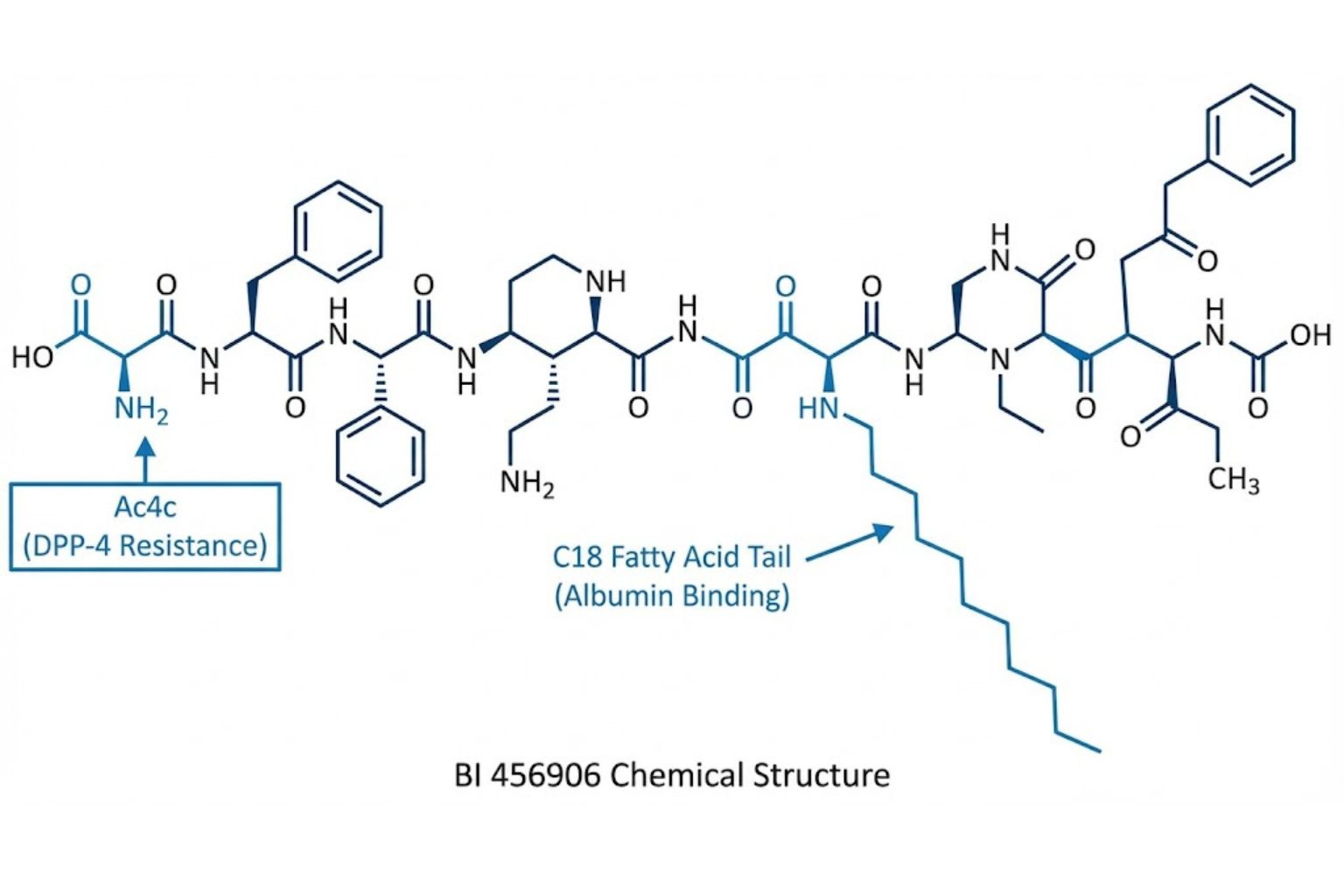
2. The Molecule: Structural Pharmacology
Survodutide is not a naturally occurring hormone. It is a synthetic peptide, chemically optimized for two critical properties: Dual Affinity and Proteolytic Stability.
The Glucagon Backbone
Unlike Tirzepatide (which utilizes a GIP-based backbone), Survodutide is derived from the glucagon amino acid sequence. This is a deliberate design choice. The native glucagon sequence has a natural affinity for the liver, which is the primary organ of interest for this specific drug.
-
Modification: The peptide backbone is modified with specific amino acid substitutions to introduce GLP-1 receptor affinity.
-
The “Balanced” Bias: Survodutide is not a 50/50 split. Pharmacological assays suggest it is biased towards GLP-1, with an affinity ratio of approximately 8:1 (GLP-1R : GCGR). This bias is a crucial safety feature, ensuring that the insulinotropic (blood sugar lowering) effects always overpower the glycogenolytic (blood sugar raising) effects of glucagon.
The C18 Fatty Acid Linker
Native peptides like GLP-1 and Glucagon have half-lives measured in minutes (approx. 2-5 minutes) because they are rapidly degraded by enzymes (DPP-4) and filtered by the kidneys.
-
The Fix: Survodutide incorporates a C18 fatty acid side chain attached via a linker.
-
Mechanism: This fatty acid tail binds non-covalently to serum albumin in the bloodstream. Albumin acts as a carrier protein, shielding the peptide from enzymatic degradation and preventing rapid renal clearance. This extends the half-life to approximately 100+ hours, allowing for once-weekly subcutaneous dosing.
DPP-4 Resistance
The N-terminal region of the peptide (the “head”) is the target for Dipeptidyl Peptidase-4 (DPP-4), the enzyme that inactivates incretins. Survodutide incorporates a non-coded amino acid, 1-aminocyclobutane-1-carboxylic acid (Ac4c), at position 2. This structural modification renders the peptide “invisible” to DPP-4 cleavage, ensuring it remains intact until it reaches its target receptors.
3. The GLP-1 Component: The Metabolic “Brake”
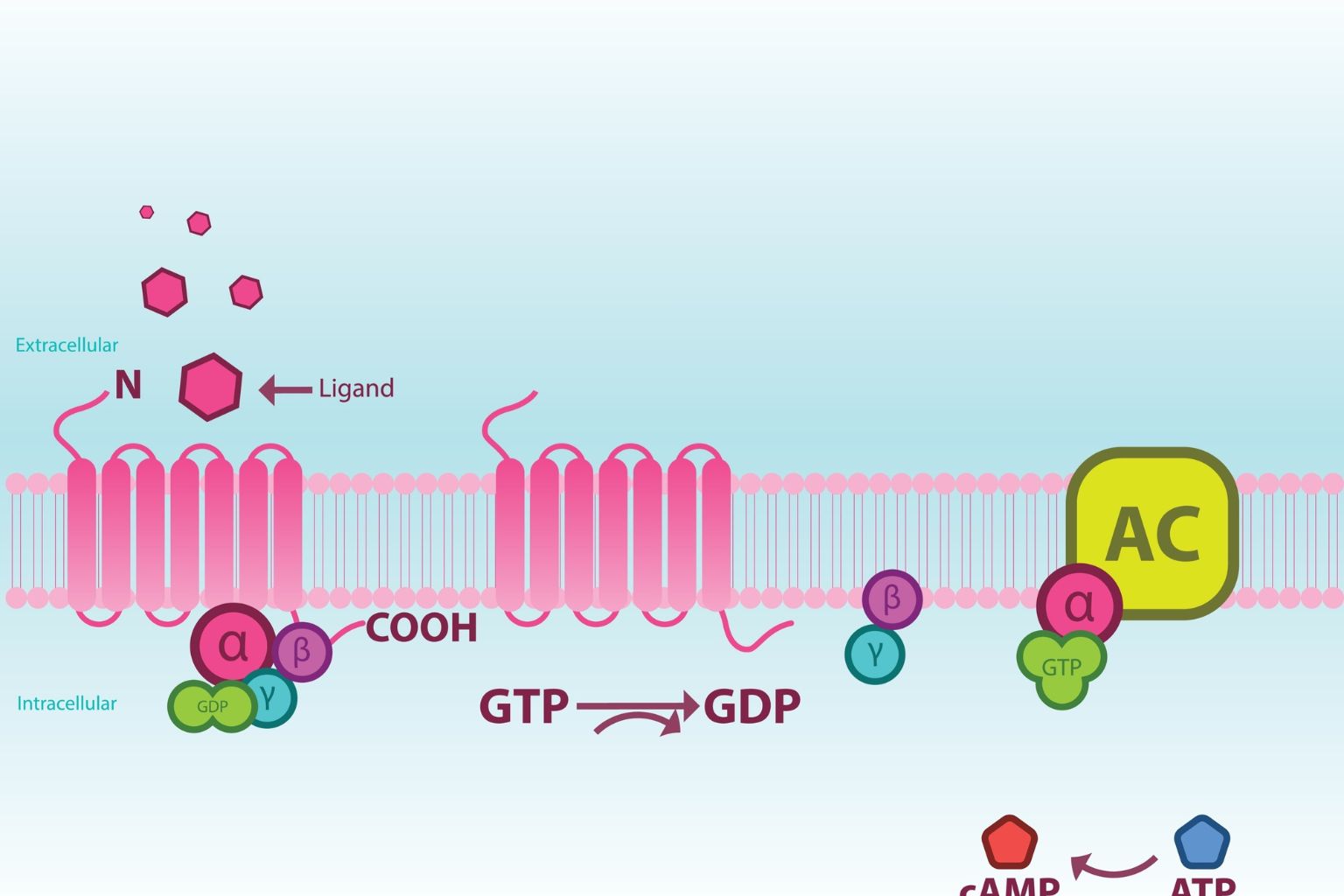
The first half of the Survodutide mechanism of action is familiar to researchers: the activation of the GLP-1 receptor. This G-protein coupled receptor (GPCR) is widely expressed in the pancreas, brain, and gastrointestinal tract.
Intracellular Signaling Cascade (Beta Cells)
When Survodutide binds to the GLP-1R on pancreatic beta cells, it triggers a classic Gs-protein coupled cascade:
-
Activation: The Gαs subunit activates the enzyme Adenylyl Cyclase (AC).
-
Second Messenger: AC converts ATP into cyclic AMP (cAMP).
-
Effectors: High levels of cAMP activate Protein Kinase A (PKA) and the exchange factor Epac2.
-
The Result: PKA closes ATP-sensitive Potassium (K_ATP) channels and opens Voltage-Dependent Calcium Channels (VDCC). The influx of Calcium (Ca2+) triggers the exocytosis of insulin granules.
-
Significance: This insulin secretion is glucose-dependent. It only happens when glucose is high, minimizing the risk of hypoglycemia.
-
Central Nervous System (The “Satiety” Signal)
Survodutide crosses the blood-brain barrier (or acts on circumventricular organs like the area postrema) to engage GLP-1 receptors in the Hypothalamus (specifically the Arcuate Nucleus) and the Nucleus of the Solitary Tract (NTS).
-
POMC Neurons: It stimulates Pro-opiomelanocortin (POMC) neurons, which release alpha-MSH to suppress appetite (anorexigenic).
-
NPY/AgRP Neurons: It inhibits Neuropeptide Y (NPY) and Agouti-Related Peptide (AgRP) neurons, which normally stimulate hunger (orexigenic).
-
The Feeling: The subject experiences “early satiety” (fullness) and reduced “food noise” (craving).
Gastric Motility
GLP-1 agonism inhibits the vagal nerve outflow to the stomach. This slows Gastric Emptying.
-
Effect: Nutrients enter the small intestine more slowly, preventing post-prandial glucose spikes and physically prolonging the sensation of stomach fullness.
4. The Glucagon (GCGR) Component: The Metabolic “Gas”
This is the key differentiator. If GLP-1 is the brake on intake, Glucagon is the foot on the accelerator of expenditure. Historically, Glucagon was feared as a “diabetic hormone” because it raises blood sugar. However, in the context of the Survodutide mechanism of action, it is repurposed as a catabolic powerhouse.
Hepatic Lipolysis (Direct Liver Action)
The liver is the primary target of Glucagon. The GCGR is highly expressed on hepatocytes.
-
Signaling: Binding triggers the Gs-cAMP-PKA pathway within the liver cell.
-
Lipid Mobilization: PKA phosphorylates key enzymes involved in lipid metabolism, specifically Hormone-Sensitive Lipase (HSL) and Perilipin.
-
Beta-Oxidation: This shifts the liver’s metabolism from “storage mode” (Lipogenesis) to “burn mode” (Beta-Oxidation). The liver begins to aggressively break down stored triglycerides into free fatty acids and ketone bodies to be used for fuel.
-
Significance: This is why Survodutide is superior to Tirzepatide for liver fat reduction. It doesn’t just wait for the patient to lose weight; it chemically instructs the liver to burn its own fat stores.
-
Thermogenesis (Energy Expenditure)
Glucagon has a recognized thermogenic effect. It stimulates Brown Adipose Tissue (BAT) and promotes the “browning” of white adipose tissue (Beige Fat).
-
UCP-1 Activation: Glucagon signaling upregulates Uncoupling Protein 1 (UCP-1) in the mitochondria of fat cells.
-
The Uncoupling: Normally, mitochondria use the proton gradient to make ATP (energy). UCP-1 creates a “leak” in this gradient. The energy is released as HEAT instead of ATP.
-
The Result: The basal metabolic rate (BMR) increases. The subject burns more calories at rest. In animal models, Survodutide-treated subjects lose weight even when pair-fed (eating the same amount) as controls, proving that the weight loss is driven by increased expenditure, not just reduced intake.
5. Synergy: Why 1+1=3
The genius of the Survodutide mechanism of action lies in how these two opposing forces stabilize each other.
The Glucose Buffer
-
The Risk: Glucagon stimulates Glycogenolysis (breakdown of glycogen to glucose) and Gluconeogenesis (making new glucose) in the liver. In isolation, this would cause hyperglycemia (high blood sugar).
-
The Solution: The GLP-1 component stimulates robust Insulin Secretion. Insulin is the most potent inhibitor of hepatic glucose production.
-
The Balance: The strong insulin response (driven by GLP-1) completely cancels out the hyperglycemic risk of the Glucagon. The subject gets the fat-burning benefits of Glucagon without the diabetes risk. In fact, HbA1c drops significantly during Survodutide treatment.
The Lipid-Satiety Loop
-
Glucagon reduces lipids in the liver.
-
GLP-1 reduces lipids in the diet (via reduced intake).
-
Together, they attack visceral adipose tissue from both ends: Input Restriction and Output Acceleration. This leads to rapid mobilization of the most dangerous fat depots (visceral and hepatic), which are metabolically more active than subcutaneous fat.
6. Impact on NASH/MASH: The Fibrosis Breakthrough
Metabolic dysfunction-associated steatohepatitis (MASH) is the holy grail of metabolic drug development. It is characterized by three stages: Steatosis (Fat), Inflammation (Ballooning), and Fibrosis (Scarring). Survodutide has shown Phase 2 results (83% resolution) that outperform almost any other agent.
Mechanism of Anti-Fibrosis
How does Survodutide reduce scarring?
-
De-Lipidation: By aggressively clearing liver fat (via the Glucagon pathway described above), the “toxic fuel” that drives inflammation is removed. Lipotoxicity is the primary driver of hepatocyte injury.
-
Mitochondrial Biogenesis: Glucagon signaling improves mitochondrial turnover (Mitophagy). Old, damaged mitochondria are replaced by healthy ones, reducing Oxidative Stress (ROS).
-
Hepatic Stellate Cells (HSC): These are the cells that make collagen (scar tissue). While Survodutide targets hepatocytes, the reduction in inflammatory signaling (TNF-alpha, IL-6) from healthy hepatocytes causes activated HSCs to revert to a quiescent state.
-
Direct Effect? Emerging research suggests there may be direct Glucagon receptors on HSCs that inhibit their activation, though this is still being elucidated.
-
7. The Safety Profile Explained Pharmacologically
Heart Rate (Chronotropy)
Researchers will note an increase in heart rate with Survodutide.
-
Mechanism: Glucagon receptors are present in the Sinoatrial Node (the heart’s pacemaker). Activation increases cAMP in cardiac myocytes, increasing heart rate.
-
Context: This is a known class effect of glucagon-based agonists. While usually benign, it is the reason for slow dose titration.
Nausea (The GLP-1 Tax)
The nausea is primarily driven by the Area Postrema activation. However, the Glucagon component may also relax the smooth muscle of the pyloric sphincter, potentially modulating the gastric delaying effect of GLP-1. The precise interaction here contributes to the unique tolerability profile of the drug.
8.The Future of Dual Agonism
The Survodutide mechanism of action proves that we can “hack” the body’s energy equation. By combining the “Brake” (GLP-1) and the “Gas” (Glucagon), Survodutide offers a comprehensive solution to Metabolic Syndrome. It doesn’t just starve the fat; it burns it.
For the researcher, Survodutide is more than a weight loss drug; it is a probe into the plasticity of human metabolism. It challenges the dogma that Glucagon is “bad” and establishes a new frontier where Energy Expenditure is a viable therapeutic target alongside appetite suppression.
As we move into Phase 3 trials, the data derived from this molecule will likely rewrite the textbooks on how we treat the liver, the heart, and the adipose organ as a singular, interconnected system.
9. References & Further Reading
For researchers wishing to verify the pathways discussed:
-
Finan, B., et al. (2015). A rationally designed monomeric peptide triagonist corrects obesity and diabetes in rodents. Nature Medicine. (Foundational paper on poly-agonism concepts).
-
Zimmermann, T., et al. (2022). BI 456906: Discovery and preclinical pharmacology of a novel GCGR/GLP-1R dual agonist. Molecular Metabolism. (The specific discovery paper for Survodutide).
-
Drucker, D. J. (2018). Mechanisms of Action and Therapeutic Application of Glucagon-like Peptide-1. Cell Metabolism.
